Intestinal Polyps
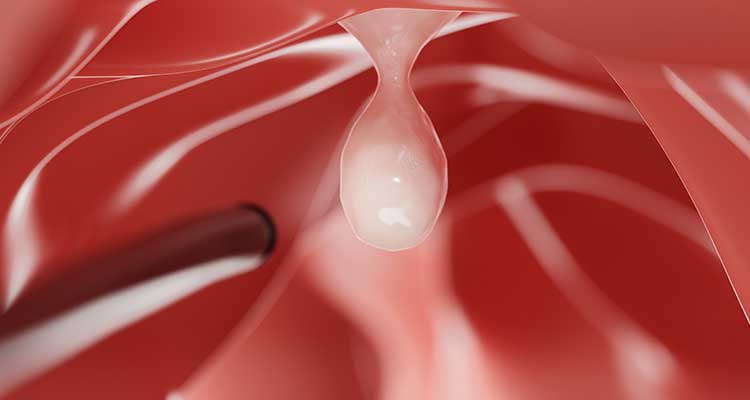
Intestinal polyps are lesions that protrude from the inner wall of the intestine into its lumen. They are more common in the colon and rectum but may occur in any segment of the digestive tract, such as the small intestine, stomach or oesophagus. These lesions vary in number, size, shape and histological type. Most polyps are isolated, but some individuals develop multiple polyps, particularly in hereditary conditions known as intestinal polyposis syndromes.
The clinical relevance of intestinal polyps lies in their potential for malignant transformation: some adenomas may progress to colorectal cancer over several years, with the risk increasing according to lesion size. In contrast, hyperplastic polyps are usually small, located in the distal colon and have no malignant potential.
Most common symptoms:
- Most patients are asymptomatic, especially when polyps are small;
- Occult blood in the stool, detectable in screening tests;
- Rare changes in bowel habits (diarrhoea or constipation);
- Anaemia resulting from intestinal blood loss;
- Severe diarrhoea in cases of large villous adenomas, usually located in the rectum or sigmoid colon.
Diagnosis is usually made by colonoscopy, which allows both identification and removal of polyps (polypectomy), thereby preventing progression to cancer. Endoscopic removal is safe and painless.
Currently, even polyps with malignant transformation, by definition early-stage colon tumours, can often be treated using advanced endoscopic techniques, such as submucosal or intermuscular dissection, avoiding the need for surgery, which is more invasive. Surgery is required only in very rare cases, usually when there are features that contraindicate endoscopic removal.
Risk factors and prevention:
- Genetic predisposition and family history of polyps;
- Diet high in fat and low in fibre, fruits and vegetables;
- Excessive alcohol consumption and smoking;
- Obesity and sedentary lifestyle;
- Hereditary syndromes, such as familial adenomatous polyposis, Gardner syndrome, Turcot syndrome, Peutz–Jeghers syndrome and Lynch syndrome;
- Use of aspirin and other non-steroidal anti-inflammatory drugs, as well as a calcium-rich diet, may have a protective effect.
After removal, polyps are analysed histologically to confirm their benign nature. Follow-up is determined by the number, size and histological type of the removed polyps, with surveillance colonoscopy generally recommended every 3 to 5 years, or at shorter intervals in specific situations. Screening and endoscopic removal of polyps are therefore fundamental in the prevention of colorectal cancer, ensuring that precursor lesions are treated before becoming malignant.
- Dra. Ana Margarida Vieira
- Dr. André Sancho Ramos
- Dr. Bruno Peixe
- Dra. Helena Tavares de Sousa
- Dra. Maria Margarida Sampaio
- Dra. Patrícia Queirós
- Dra. Ana Rita Herculano
- Dr. André Sancho Ramos
- Dr. Diamantino Sousa
- Dr. Francisco Açucena
- Dr. Horácio Guerreiro
- Dr. Mário César
- Dr. Horácio Guerreiro
- Dra. Carla Sousa Andrade
- Dra. Isabel Jardim
- Dr. Luís Jasmins
- Dr. Nuno Ladeira
- Dra. Rosa Neto da Silva
- Dr. Vítor Magno Pereira
- Dra. Carla Sousa Andrade
- Dra. Isabel Jardim
- Dr. Luís Jasmins
- Dr. Nuno Ladeira
- Dra. Rosa Neto da Silva








